Proposed Rule Data Modeling Available

CIGNA
Cigna Healthcare® has announced a new reimbursement policy—Evaluation and Management Coding Accuracy (R49)—which will take effect for dates of service on or after October 1, 2025. This policy targets high-level E/M codes (99204–99205, 99214–99215, and 99244–99245) and is designed to ensure alignment with AMA evaluation and management (E/M) documentation guidelines. Under the new policy, Cigna will conduct periodic claim reviews and may downcode services by one level if the submitted documentation does not support the billed level. Providers with consistently accurate documentation may be removed from future reviews. If a claim is adjusted, providers may request reconsideration by submitting the full medical record for the encounter. If the documentation justifies the original code, the claim will be reprocessed. An appeal process remains available for further disputes. Practices should begin reviewing internal documentation and billing practices now to minimize disruption and avoid potential reimbursement reductions.
Understanding Contract Law and When a Contract is Voidable
Under the Restatement (Second) of Contracts, a seemingly valid agreement can still be set aside when the law deems it voidable, meaning the disadvantaged party alone holds the power to rescind. This power arises when the quality of assent is impaired or when public policy protects a vulnerable promisor. First, the Restatement recognizes lack of legal capacity (§§ 12–16): contracts made by minors, those suffering mental incapacity, the intoxicated, or persons under guardianship are enforceable only at the competent party’s option because the law presumes their assent is unreliable. Second, mistake can undermine assent. A mutual mistake of a basic assumption that materially affects the bargain (§ 152) allows either party to avoid the contract unless the agreement or the circumstances allocate that risk to the party seeking relief; a unilateral mistake (§ 153) also supports avoidance when enforcement would be unconscionable or the other party had reason to know of the error.
The doctrine of misrepresentation (§§ 159–164) likewise makes a contract voidable whenever a party’s manifestation of assent is induced by a fraudulent or even simply material misstatement of fact and the reliance is justifiable. Here, the innocent party may rescind, demand restitution, or affirm the contract and sue for damages; deliberate fraud defeats any attempt to shield the wrongdoer with non-reliance or exclusive-remedy clauses. Assent procured by duress (§§ 174–176)—an improper threat that leaves no reasonable alternative—and by undue influence (§ 177)—unfair persuasion exerted through a position of dominance or trust—creates the same avoidance right. In each setting, the contract is binding on the other side but remains contingent until the protected party elects whether to disaffirm.
Exercising the power of avoidance requires timely action and restoration of any benefits received, consistent with restitution principles (§§ 376, 384). If the party delays unreasonably after discovering the defect or otherwise manifests an intent to proceed, courts treat that conduct as ratification, converting the voidable agreement into a fully enforceable one. Conversely, prompt rescission unwinds the transaction and returns the parties to the status quo ante. Thus, capacity defects, mistake, misrepresentation, duress, and undue influence each supply a legal “off switch” that vests in the injured party alone—illustrating the Restatement’s central theme that genuine, informed, and voluntary assent is the cornerstone of contractual obligation.
EXAMPLE:
When a revenue-cycle firm pitches prospective healthcare clients with glossy spreadsheets promising, say, “$750 000 in new annual collections” or a “15 % lift in payer yield,” those figures function exactly like the inflated earnings projections that have repeatedly triggered rescission in Delaware and federal courts. Under Restatement (Second) of Contracts § 164, a contract is voidable if a party’s assent is induced by a fraudulent or even merely material misrepresentation on which it justifiably relies. Courts treat near-term financial forecasts as actionable statements of fact when the speaker knows—or recklessly disregards—that they lack a reasonable basis: in Abry Partners v.
F&W Acquisition the buyer was allowed to unwind a stock-purchase agreement after discovering revenue figures the seller had padded to clinch the deal, and Prairie Capital III v. Double E Holding let fraud claims proceed where working-capital projections fed to the buyer proved wildly off the mark.
Even small operators prevail: franchisees in Bans Pasta LLC v. Mirko Franchising stated a rescission claim when the franchisor’s spreadsheets guaranteed six-figure profits that never materialized. By analogy, a hospital or oncology group that signs an RCM agreement because the vendor touted specific, superior reimbursement results—and then sees no such improvement
—can invoke the same doctrine to terminate the contract, demand restitution, or affirm and sue for benefit-of-the-bargain damages. Anti-reliance or exclusive- remedy clauses will not save the billing company if the court finds the revenue projections were knowingly or recklessly false, because public-policy limits prevent parties from insulating outright fraud. In short, promising “more money” without a defensible factual foundation is more than marketing puff—it is a misrepresentation that gives the client a clear legal pathway to walk away and recover losses.
Billing Company and Third Party Software
We’ve received a surge of calls and emails from practices currently using third- party billing companies—and the concerns are piling up. Let’s be clear: there’s nothing inherently wrong with outsourcing billing. In many cases this actually is more cost effective and can be more accurate. But we are now seeing a growing pattern that should give everyone pause.
More and more billing companies are pushing their own coding software or third- party applications. Again, on the surface, that’s not necessarily a problem. But here’s what you need to ask:
Is this software a replacement for manual coding or an add-on to existing services?
Because if they’re already charging you for coding services, then promoting a software tool raises real questions—about conflicts of interest, staffing gaps, and what you’re truly paying for.
Here’s the larger issue: these coding programs are not recovering lost revenue. Despite flashy claims and sales pitches, they do not identify missed charges or underpayments in any meaningful way. Why? Because the data and insights needed to find that money live deeper in the claims lifecycle—after the claim is coded. This includes adjudication, denials, 835 transactions, and remittance activity.
Departmental-level software cannot do this alone. Your claims have already passed through scrubbing and internal rules engines. So if someone tells you that missed revenue is sitting untouched at the departmental coding level— they’re either misunderstanding the process or intentionally oversimplifying it. To be fair, these tools can be helpful for reconciliation—they help confirm whether something was captured and aligned. But let’s not pretend they’re the solution to deeper revenue cycle problems.
So why would a billing company promote coding software in the first place? Maybe they’re incentivized. Maybe they have a vested interest.
Maybe they’re under-resourced and need the software to fill staffing gaps. Or maybe they see a revenue opportunity by reselling tools.
Either way, you deserve transparency.
You should know the relationship and the exposure of your data.
Ask hard questions. Be vigilant.
And be especially wary of promises like:
“We guarantee a dollar amount of recovery.”
“It’s low-cost this year… but in year two the price jumps.”
These models are not designed with your long-term success in mind. Revenue cycle success is never just about software. It’s about transparency, accountability, and full visibility across your claims—from scheduling to payment.
If you want help understanding what’s really happening with your reimbursement, we’re here to walk you through it—no gimmicks, no shortcuts, and no hidden markups.
PT and OT
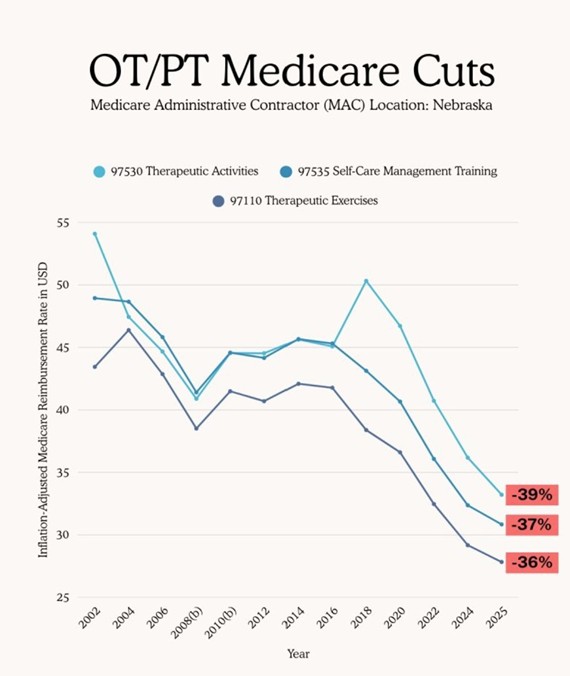
Health Tech
The Biden administration has launched a new public-private data-sharing initiative to create a “digital health ecosystem,” bringing together over 60 companies—including tech giants like Apple, Amazon, OpenAI, and Google, as well as health insurers and app developers—to facilitate the seamless flow of patient data between consumers and providers. While the goal is to increase patient access and modernize health records through AI tools and digital platforms, the initiative raises significant privacy concerns.
Many participating companies are not covered by HIPAA, instead falling under a patchwork of state and federal consumer privacy laws that vary in scope and enforcement. Legal experts warn this fragmented regulatory landscape could confuse consumers and leave gaps in health data protections, particularly around sensitive information like reproductive or gender-affirming care.
Federal regulators, including HHS and the FTC, say enforcement will focus on transparency, breach notifications, and honoring privacy commitments.
However, legal experts caution that companies must be able to deliver on any privacy and security promises, or face potential scrutiny under laws like the FTC Act or new state statutes such as Washington’s My Health, My Data Act. State attorneys general, including in Texas and California, are already ramping up enforcement efforts.
Though the initiative is voluntary, the varied legal obligations among participants—from HIPAA to FTC and state-specific rules—mean that navigating compliance will be complex. Ultimately, companies must not only align with evolving regulations but also build and maintain consumer trust in how they handle and share sensitive health data. With a 2026 timeline for deliverables, including digital tools and interoperable data exchanges, the initiative’s success may hinge as much on its privacy safeguards as its technological ambition.
Arkansas Set To Block
Arkansas Governor Sarah Huckabee Sanders is opposing steep health insurance premium increases proposed by insurers like Centene Corp. and Blue Cross Blue Shield, some of which exceed 50%, according to the state’s insurance department. Sanders called on regulators to reject the hikes, placing blame on insurers, though much of the increase is driven by broader national issues—rising medical costs and uncertainty over whether congressional Republicans will extend federal subsidies for Affordable Care Act (ACA) plans.
If the subsidies lapse, healthier individuals may leave the market, causing premiums to rise further due to a sicker insurance pool. Insurers are also adjusting for increased costs and federal crackdowns on enrollment fraud. Nationally, ACA insurers are seeking a median premium increase of 18%, more than double last year’s rate. Major insurers, including Centene, Cigna, and UnitedHealth, are seeking increases of 20–30% as they struggle with rising medical expenses and lower-than-expected earnings.
Bridge Unveils First of Its Kind Program for Radiation Oncology: Uncovering Seven Figure Dollars
Is Your Radiation Oncology Department Leaving Millions on the Table?
Bridge Revenue Solutions Uncovers and Fixes the Hidden Gaps
Radiation oncology departments face complex revenue challenges that standard revenue cycle management (RCM) vendors often fail to address. As margins tighten and the pressure to optimize increases, Bridge Revenue Solutions offers a powerful answer: a specialized, data-driven approach that transforms how radiation oncology departments operate and bill.
Bridge’s Assessment Program recently uncovered $4.2 million in missed annual revenue at a 16-site oncology network—revealing that 23% of charges were either undercoded or never submitted. The culprit? Disconnected systems, unstandardized documentation, and broken workflows across billing, clinical, and administrative teams.
That’s why Bridge offers far more than just outsourced RCM—it delivers fractional revenue integrity and full integration with clinical, operational, and Central Business Office (CBO) functions. From intake through charge capture and appeals, Bridge embeds its team alongside yours to build coordinated, compliant, and high-performing revenue processes.
Their services span 14 critical areas, including authorization workflows, charge reconciliation, credit balance management, and payer-specific clean claim editing. Weekly standing meetings, workflow integration across EPIC, ARIA, MOSAIQ, and a 6–12 month engagement timeline ensure sustainable improvements—not just short-term fixes.
What sets Bridge apart is shared ownership. Their embedded teams train and equip internal staff, ensuring long-term success even after engagement ends. And they don’t just chase claims—they fix the systems causing the breakdowns in the first place.
Bridge’s proactive cross-checks and dashboards help reduce costly errors like treatment plan changes that go uncommunicated post-authorization—one of the top causes of preventable denials.
If you’re ready to recover lost revenue, reduce denials, and create alignment across your RCM and clinical teams, Bridge Revenue Solutions is your partner in building a future-proof radiation oncology service line.
Price Transparency
wo U.S. senators, John Hickenlooper and Roger Marshall, MD, have introduced the Patients Deserve Price Tags Act, a bipartisan bill aimed at dramatically improving healthcare price transparency. The legislation would mandate that health plans and providers publicly share actual negotiated rates and cash prices—not estimates—in machine-readable formats. Hospitals would also be required to post the real prices of 300 shoppable services through the end of 2026, after which the rule would apply to all shoppable services.
Additionally, the bill would require itemized patient bills or bundled all-in pricing options, along with explanations of benefits for patients. Failure to comply with these requirements could carry steep penalties, with fines tiered by hospital size. For instance, hospitals with over 500 beds could face daily fines up to
$35 per bed after a year of noncompliance. Furthermore, hospitals found to be persistently noncompliant—defined as two or more violations within a year— could be subject to additional penalties ranging from $500,000 to $10 million, depending on their size.
This proposed legislation builds on a broader push for price transparency that began with a 2020 executive order by President Donald Trump. CMS updated its hospital price transparency rules in May 2025 to clarify that hospitals must post actual prices, not estimates. Despite these measures, compliance remains inconsistent. CMS has fined only 27 hospitals since enforcement began in 2022.
Senator Marshall emphasized the importance of transparency, stating, “Patients should know the price of the service they need before they make any decisions.” If passed, the bill would strengthen enforcement and provide patients with clearer, upfront cost information—potentially reshaping the financial landscape for hospitals nationwide.
IGRT by the Numbers
The 2026 Proposed Rule introduces sweeping changes for radiation oncology— most notably, the deletion of imaging codes G6002, 77014, and G6017. While many in the field are frustrated by this move, it’s important to understand the broader context. These codes weren’t erased without recourse—they were consolidated into CPT 77387. Although reimbursement for 77387 is currently set at just $37 (far below the over $100 previously seen for 77014), this shift should still be seen as a strategic win.
Consider this: A national review of 2024 claims data from 5,400 radiation oncologists (incomplete) revealed 4.36 million units of 77014 billed, totaling nearly $700 million in charges, with an average charge of $387. IGRT is performed daily on over 70% of patients, and historically, such high utilization often leads CMS to delete and fully bundle these services—eliminating professional reimbursement altogether. The fact that we retained standalone IGRT codes for the professional component is significant and represents a major policy win for the field.
PhRMA Fall Short
A federal court in Texas has again rejected the pharmaceutical industry’s attempt to block Medicare’s drug price negotiation program, marking the third legal defeat for drugmakers in just two days.
On Thursday, Judge David Alan Ezra of the U.S. District Court for the Western District of Texas ruled against the Pharmaceutical Research and Manufacturers of America (PhRMA) and its co-plaintiffs—the National Infusion Center Association (NICA) and the Global Colon Cancer Association—dismissing their constitutional challenges to the Medicare Drug Price Negotiation Program created under the Inflation Reduction Act (IRA). Judge Ezra found that the plaintiffs failed to demonstrate any deprivation of property rights or interference with their operations. “The Program does not seize providers’ facilities or otherwise interfere with their processes for administering Medicare-reimbursed drugs,” he wrote. He emphasized that Medicare is functioning as a market participant, not a coercive regulator, merely setting the terms under which it will pay for certain drugs. Manufacturers are not entitled to force the government to buy drugs on their terms.
PhRMA spokesperson Sarah Ryan said the group strongly disagrees with the ruling and maintains that the IRA’s price-setting provisions are unconstitutional. This is the third federal court ruling in less than 48 hours upholding the legality of the program:
The U.S. Court of Appeals for the Second Circuit rejected similar claims brought by Boehringer Ingelheim.
The Sixth Circuit dismissed a challenge by the U.S. Chamber of Commerce and affiliates, citing lack of standing.
Originally, Judge Ezra dismissed the case in February 2024 for lack of jurisdiction, stating that claims related to Medicare must first go through administrative channels. However, the Fifth Circuit reversed that in September 2024, ruling that the case could proceed because the claims stem from the IRA, not the Medicare Act.
The legal challenges argued that the negotiation program violates the separation of powers, Fifth Amendment due process, and the Eighth Amendment’s excessive fines clause. The plaintiffs also claimed the program would financially harm NICA’s members through lower Medicare Part B and D reimbursements.
However, with this latest decision, legal momentum is clearly shifting in favor of the federal government. Patients for Affordable Drugs executive director Merith Basey called the ruling a “win for patients nationwide,” adding that “Pharma has been dealt three decisive blows,” and reaffirming that “Big Pharma’s legal arguments are meritless.”
AETNA
Aetna, the health insurance arm of CVS Health, plans to terminate nearly 90 Medicare Advantage (MA) plans across 34 states in 2026, according to a notice shared with third-party brokers this week. The majority of these affected plans are PPOs. Additionally, beginning September 1, 2025, Aetna will stop paying commissions to brokers for enrolling new members in these commission- excluded plans. However, Aetna has not officially announced specific details regarding its overall Medicare Advantage offerings for 2026.
These strategic reductions come amid a broader industry pullback from Medicare Advantage, driven by rising medical costs and shrinking margins. CVS Health, Aetna’s parent company, has nonetheless shown notable financial improvement. In the second quarter of 2025, CVS outperformed expectations, prompting an upward revision of its full-year adjusted earnings guidance to between $6.30 and $6.40 per share, up from the earlier $6.00–$6.20 range.
This marks at least the third consecutive quarter of earnings beats for CVS. Within the Aetna insurance division, margin improvements are becoming evident. Aetna’s medical loss ratio (MLR) came in at 89.9%, outperforming analyst expectations of around 91%, signaling better cost control. The company also disclosed plans to reprice approximately half of its group Medicare Advantage plans for 2026 as part of its broader effort to restore profitability.
In sum, while Aetna is trimming its MA offerings—including broker commission changes and PPO reductions—the insurer is simultaneously executing a broader turnaround through more disciplined pricing, cost controls, and strategic repricing of key plan portfolios.
RPM and RTM: 2026 Proposed Rule
Bridge Oncology’s Legal & Technology Arm: 2026 Proposed RPM and RTM CPT Codes Overview
The 2026 Proposed CPT Codes for Remote Physiologic Monitoring (RPM) and Remote Therapeutic Monitoring (RTM) introduce key changes that will impact reimbursement models, workflow, and vendor partnerships across the healthcare industry. Key highlights include:
New Codes and Reimbursement Rates:
99XX4 (Remote Monitoring of Physiologic Parameters) is proposed at $47.70.
99XX5 (RPM Treatment Management, first 10 minutes) at $25.53.
98XX4-98XX7 (RTM for various therapeutic applications) range in reimbursement from contractor-priced to $39.97.
Key Issues and Stakeholder Considerations:
Contractor Pricing for Certain RTM Device Supply Codes: CMS is proposing contractor pricing for RTM device supply codes 98XX4 and 98976, creating local variability in payment amounts and reducing predictability for vendors.
Billing Period Mismatch: A persistent issue remains with the disconnect between the 30-day period for device supply codes and the calendar-month basis for treatment management codes, complicating billing and increasing the risk of denials.
Reimbursement Discrepancy Between RPM and RTM: The proposed rule introduces a payment disparity between RPM and RTM device supplies, notably for musculoskeletal monitoring (RTM), potentially disincentivizing RTM adoption. Simplified Device Supply Reimbursement: Proposed equal valuation for both 2–15-day and 16–30-day device supply codes could simplify billing and stabilize vendor pricing.
Impact of Time-Based Scaling: For treatment management, the introduction of 10-minute codes (99XX5, 98XX7) reflects CMS’s move toward fee-for-service models, resulting in lower reimbursement compared to longer-duration codes, thereby creating pressure on vendors serving low-engagement patients.
Strategic Opportunities for Stakeholders:
Advocacy: Stakeholders should comment on critical areas such as the RPM-RTM reimbursement discrepancy, alignment of billing periods, and the impact of contractor pricing on reimbursement predictability.
Vendor Strategy: Vendors may consider modular service models that align with shorter-duration treatment management codes, and implement clearer billing documentation to withstand increased scrutiny.
Final Thoughts: As CMS continues to normalize remote monitoring, providers, and vendors must navigate the evolving landscape by engaging with the comment process and adjusting their business models for the upcoming reimbursement shifts.
MedLever
As the White House and CMS push forward with the Health Tech Ecosystem Initiative, the future of healthcare will be shaped by seamless digital tools that improve patient care and drive interoperability. In this rapidly evolving landscape, radiation oncology must not be left behind. A clear leader has emerged—MedLever.
MedLever is revolutionizing the way radiation oncology integrates with the broader healthcare ecosystem. Unlike many imitating companies that are still “building the plane while flying,” MedLever has already charted its course. This innovative platform is not just reactive; it’s proactive, designed specifically for radiation oncology and proven across cancer centers and health systems.
With MedLever, outdated paper-based and manual processes are a thing of the past. The platform integrates seamlessly across Electronic Health Records (EHR), Oncology Information Systems (OIS), and ancillary systems, ensuring no more data silos or delays in care.
MedLever is at the forefront of CMS interoperability mandates for 2026 and beyond, providing an intelligent, patient-friendly interface that unlocks automation and data-driven coordination. By eliminating inefficiencies, MedLever empowers oncology teams to deliver faster, smarter, and cleaner operations—critical for meeting the demands of value-based care.
In an industry increasingly driven by digital health, MedLever stands apart, not just as a tool, but as the key to unlocking better patient outcomes. It’s not just about keeping up; it’s about leading the charge. Radiation oncology now has the platform to thrive in the digital age—without the growing pains of unproven systems. MedLever is the future, and it’s already here.
G2211
Determining whether HCPCS code G2211 can be billed when a patient sees a different physician or practitioner within the same group practice, even
colleagues in the same specialty, presents an interesting coding challenge. The key consideration revolves around whether the new provider serves as the “continuing focal point for all needed services or provides ongoing care for that complex or serious single condition.”
Expert analysis by specialists like Terry is crucial in breaking down these nuances to ensure accurate coding for the G2211 complexity add-on. The code’s intent is to recognize the inherent complexity of visits that are part of a longitudinal patient-provider relationship, either where the practitioner is the primary point of contact for all healthcare needs, or where they manage a single, serious, or complex condition over time.
When a patient transitions to a new provider within the same group, even in the same specialty, the question arises whether the new provider has established or intends to establish the same level of consistent, ongoing care that would justify billing G2211. This requires careful consideration of the documentation and the nature of the relationship being built with the new practitioner.
Summary:
G2211 Billing Criteria: HCPCS code G2211 is an add-on code that reflects the complexity of office/outpatient evaluation and management (E/M) visits. It is intended to be billed in addition to E/M codes (CPT 99202–99205, 99211–99215) when the provider serves as the continuing focal point for all needed healthcare services or provides ongoing care for a single, serious, or complex condition.
Team-Based Care Considerations: In group practices, even if a patient sees a different provider within the same specialty, G2211 may still be appropriate if the new provider assumes or continues the role of the continuing focal point for the patient’s care. This is particularly relevant in team-based care models where multiple providers collaborate on managing a patient’s complex or serious condition.
Documentation Requirements: Accurate and thorough documentation is essential to support the billing of G2211. The medical record should clearly indicate the provider’s role in the ongoing management of the patient’s condition, including assessments, care plans, and follow-up arrangements.
Medicare Reimbursement: As of January 1, 2024, Medicare reimburses G2211 at a national rate of approximately $16.05. However, reimbursement rates may vary based on geographic location and other factors.
Modifier Considerations: G2211 cannot be billed on the same day as an E/M service with modifier -25, except in certain cases starting January 1, 2025, when the E/M service is reported with an Annual Wellness Visit (AWV), vaccine administration, or any Medicare Part B preventive service.
In conclusion, when a patient sees a different provider within the same group practice, billing G2211 is appropriate if the new provider assumes or continues
the role of the continuing focal point for the patient’s care. This decision should be supported by comprehensive documentation that reflects the ongoing, longitudinal nature of the patient-provider relationship.


